The gift of speech is priceless
Patients with tracheostomies and laryngectomies can have problems vocalising and communicating, but strategies exist to help. Imagine waking up from a critical illness, confused and frightened, attached to a ventilator with a cuff-inflated tracheostomy tube. Patients can speak earlier with aggressive, multidisciplinary assessment and interventions to get the cuff down as soon as possible. Techniques such as Above Cuff Vocalisation (ACV) can help patients communicate safely and effectively if the cuff cannot be deflated. Our next research projects are looking at ways that improving laryngeal airflow can help to rehabilitate the larynx, especially after critical illness.
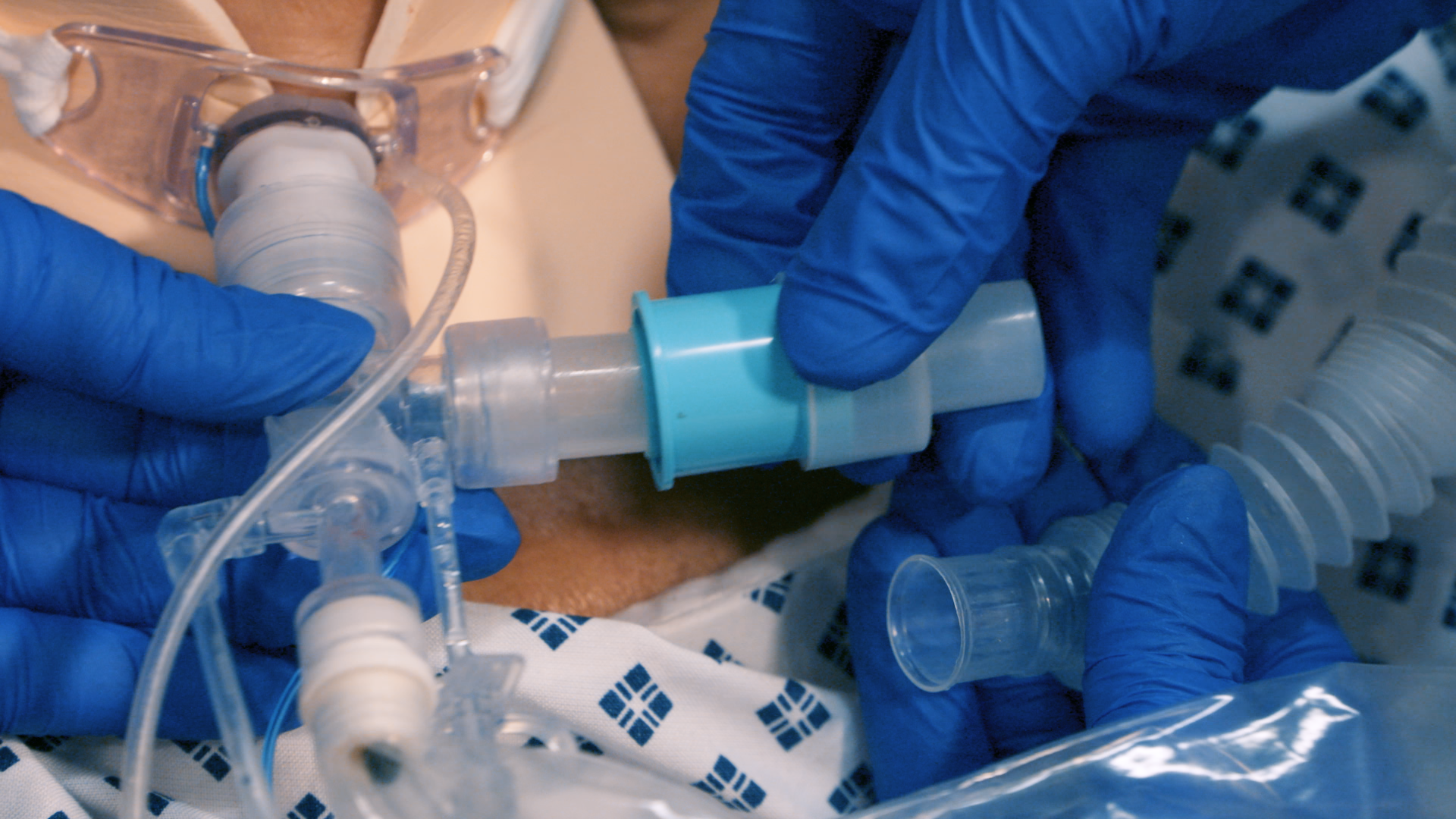
Speaking valves, alternative communication techniques and methods of vocalising following laryngectomy are also explained in this section.
Speech & Language Therapists (or Pathologists, depending on which country you work in) have a key role to play as part of the Multidisciplinary Tracheostomy Team, along with (Respiratory) Physiotherapists, Nursing, Medical and other specialist staff. The patient and their family are also a key part of this teamwork. Our publications help explain these roles and how we can work together to get our patients talking.
- Bonvento et al. Role of the MDT in the care of the tracheostomy patient. Journal of Multidisciplinary Healthcare. 2017;10:391-8
- McGrath & Wallace. The UK NTSP and the role of speech and language therapists. Current Opinion in Otolaryngology - Head & Neck Surgery. 2014;22(3):181-7.